Behavioral Disconnection Syndrome Manifesting as Combined Mania and Visual-Auditory Hallucinations Secondary to Isolated Right Thalamic Hemorrhage
Damage to the thalamus can contribute to the phenomenon of diaschisis manifesting as various behavioral symptoms. We present the case of a 55-year-old man who presented with acute mania and late-onset combined visual and auditory hallucinations after right thalamic hemorrhage. This is the first report, to our knowledge, of a combination of mania and visual-auditory hallucination in a patient with isolated thalamic damage. Details of all previous case reports on isolated thalamic damage presenting with mania or hallucination are provided. We propose the networks of diencephalic damage causing mania and hallucinations, which represent the behavioral disconnection syndromes.
It is challenging to localize a single lesion when neuropsychiatric symptoms are the only manifestations. The thalamus is a complex structure connecting between the brainstem and various cortical areas. Damage to the thalamus can contribute to various behavioral conditions. We report the first case, to our knowledge, of a patient who suffered from right thalamic hemorrhage presenting with combined acute mania and visual-auditory hallucinations. The case broadens the clinical approach on the behavioral disturbance secondary to focal brain lesion on the thalamus. We also systematically review the previous reports on the cases of isolated thalamic damage with mania or hallucination. Finally, we provide the proposed networks of diencephalic damage causing mania and hallucinations.
Case Report
A 55-year-old man without a previous history of psychiatric conditions or substance abuse presented with a 1-week history of acute mania. He had irritability, grandiosity, combative speech, paranoid delusion, high energy levels, decreased need for sleep, pressurized speech, euphoria, and inappropriate cheerfulness. The patient had been a mild-mannered and composed person prior to this event. Neurological examination showed no focal neurologic deficits; urine drug screen was negative; MRI showed cavernous malformation with hemorrhage involving the dorsomedial and pulvinar nucleus of the right thalamus (Figure 1); and electroencephalography was normal. Risperidone was started. At 4 months follow-up, the manic symptoms resolved, and risperidone was discontinued.
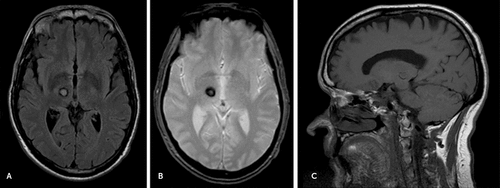
FIGURE 1. MRI Head Showing the Cavernous Malformation Hemorrhage on the Right Thalamus Involving the Dorsomedial and Pulvinar Nucleia
a The image shows A) axial view on the fluid-attenuated inversion recovery sequence; B) axial view on the gradient-echo sequence; and C) sagittal view on the T1 sequence.
One year later, he presented with acute psychosis. He had vividly visual hallucination (transient texts on his phone, unknown people and colorful airplanes). He also reported the musical hallucination that he heard pleasant classical music in particular at night. He denied any commanding or voice hallucination. He had hypnagogic visual and musical hallucinations. He has insight to the hallucinations. MRI head demonstrated stable cavernous malformation (Figure 1). Risperidone was resumed and effectively improved hallucination within a week.
Discussion
Mania
Mania after thalamic lesions has been described in a small number of patients. Symptoms of mania secondary to focal brain lesions are clinically similar to the features of primary psychiatric mania. Some features may help localizing lesions to the thalamus or differentiating from primary mania, such as hemianesthesia, hemiparesis, hypersomnolence, abnormal movement, abnormal gaze, and amnesia.
From literature review, we found 18 cases of mania (including our case) caused by isolated thalamic lesions on various thalamic nuclei, including the dorsomedial, intralaminar, pulvinar, anterior, ventrolateral, and ventromedial nuclei (Table 1). It is interesting that, in all of these cases, the lesions involved the right thalamus, with the isolated right thalamus in 72% (N=13/18) of cases and both thalami in 28% (N=5/18) of cases. The majority of patients (80%) developed mania immediately or within a few days after the damage; however, late-onset mania may occur up to many months after the events. In cases with mild symptoms, patients usually spontaneously recover without medication. In more severe cases, mood stabilizers or atypical antipsychotics are effective treatment. Even though most of the reported patients did not have recurrent mania, a minority of the cases developed hypomania or cyclic depression-mania during the follow-up period.
| Study | Sex | Age (Years) | Locations | Hemisphere | Onset | Etiologies | Manic Symptoms | Associated Symptoms | Treatment |
|---|---|---|---|---|---|---|---|---|---|
| Cummings et al.13 | Two cases | NA | Unspecified | Right | Acute | Ischemic stroke | Case 1: euphoria, talkativeness, hypersexuality, euphoric, irritable, and poor judgement | Hemisensory loss, amnesia, denial of illness, and depression (case 2) | Lithium in one case with improvement; no medication in one case |
| Case 2: euphoric, decreased need for sleep, and preoccupied with religion | |||||||||
| Gentilini et al.14 | Male | 66 | Paramedian | Right and Left | Acute | Ischemic Stroke | Hypersexuality, grandiosity, and cheerfulness | Amnesia, somnolence, and delusion | Not reported |
| Female | 47 | Paramedian | Right and Left | Acute | Ischemic stroke | Hyperphagia, euphoria, and childish behaviors | Hypersomnolence, abnormal eye movement, and depression | Not reported | |
| Male | 35 | Paramedian | Right and Left | Acute | Ischemic stroke | Hyperphagia and irritability | Amnesia | Not reported | |
| Bogousslavsky et al.6 | Female | 72 | Paramedian, dorsomedial and ventral lateral | Right | Acute | Ischemic stroke | Smiling and inappropriate laughing and jokes, logorrhea, rapid switching of ideas, lack of spontaneity, and disinhibition | Hypersomnolence, disorientation, | Not reported |
| Starkstein et al.15 | Three cases | NA | Unspecified | Right | NA | Hemorrhage and ischemic stroke | Mania (unspecified symptoms in each case) | NA | NA |
| Kulisevsky et al.16 | Female | 81 | Ventral lateral and ventromedial | Right | Acute | Ischemic stroke | Euphoria, talkativeness, grandiosity, flight of ideas, inappropriate jokes, and decreased need for sleep | Left hemichorea | Haloperidol with improvement after 4 weeks |
| McGilchrist et al.17 | Male | 43 | Paramedian | Right and Left | Acute | Ischemic stroke | Cyclic elation, hypersexuality, hyperphagia, flight of ideas, and decreased need for sleep | Hypersomnolence, cyclical apathy and depression | Not reported |
| Daum et al.18 | NA | 64 | Anterior | Right | Acute | Ischemic Stroke | Hypersexuality, talkativeness, irritability, mood fluctuation, and verbal aggression | Amnesia | Not reported |
| Vuilleumier et al.19 | Male | 63 | Unspecified | Right | Acute | Ischemic stroke | Mania episode followed by hypomania | Prosopoaffective agnosia | Not reported |
| Leibson20 | Male | 53 | Unspecified | Right | Acute | Hemorrhage | Talkativeness, cheerfulness, hypersexuality, and increased energy | Anosognosia, headache and left-sided numbness and weakness, gaze problem, and hemineglect, | Resolved 10 weeks after the stroke |
| Inzelberg et al.21 | Male | 61 | Pulvinar | Right | Acute | Ischemic stroke | Euphoria, talkativeness, disinhibition, flight of ideas, hypersexuality, decreased need for sleep, and increased goal-directed activity | Left hemichorea | Haloperidol with improvement after 8 weeks |
| Benke et al.7 | Male | 38 | Dorsomedial, intralaminar and anterior | Right and Left | 4 weeks | Ischemic stroke | Logorrhea, restlessness, mood elevation, inflated self-esteem, reduced need for food and sleep, and hypersexuality | Amnesia, vertical gaze paralysis, and dysarthria | Low-dose neuroleptic with improvement after 8 weeks |
| Lopez et al8 | Male | 63 | Unspecified | Right | 5 months | Ischemic stroke | Cyclic mania | Bipolar symptoms with cyclic depression, and melancholic stupor | Risperidone, valproic acid, and quetiapine for mania |
| Routh and Hill22 | Male | 83 | Posterior | Right | 2 weeks | Hemorrhage | Aggressiveness, speech disinhibition, talkativeness, flight of ideas, and inflated self-esteem | Paranoid delusions | Olanzapine |
| Julayanont et al. (current case) | Male | 55 | Dorsomedial and pulvinar | Right | Acute | Hemorrhage | Irritability, grandiosity, combative speech, high-energy levels, decreased need for sleep, pressurized speech, euphoria, and inappropriate cheerfulness | Paranoid delusions and amnesia | Risperidone with improvement after 4 weeks |
TABLE 1. Cases With Isolated Thalamic Damage Causing Mania
Peduncular Hallucinosis
Peduncular hallucinosis classically presents with vivid visual hallucination usually with preserved insight. Midbrain damage with or without thalamic involvement is the typical origin of hallucination. Isolated thalamic lesions were rarely reported to cause this condition (Table 2). From the literature review, we found 15 cases (including our case) of hallucinations secondary to isolated thalamic damage. Even though there is no specific thalamic nucleus consistently reported to cause peduncular hallucinosis, the dorsomedial (46%, N=6/13 cases), pulvinar (31%, N=4/13 cases), and anterior (15%, N=2/15 cases) nuclei are the common locations contributing to this condition (Table 2). Unlike mania, there is no relationship between the side of diencephalic lesions and hallucinations. From 15 case reports, the lesions were on the right side in 47% (N=7/15 cases), on the left side in 47% (N=7/15 cases), and on both sides in 6% (N=1/15 case). Similar to mania, the majority of peduncular hallucinosis (66%, N=10/15 cases) occurred within the first week after damages, but late-onset can present up to a year as reported in our case. Atypical antipsychotics are the drug of choice in severe cases.
| Study | Sex | Age (Years) | Locations | Hemisphere | Etiologies | Onset | Hallucination Features | Associated Symptoms | Treatment | |
|---|---|---|---|---|---|---|---|---|---|---|
| Visual | Auditory | |||||||||
| Feinberg and Rapcsak23 | Male | 83 | Dorsomedial | Right | Ischemic stroke | Acute | Animals in his house (flying birds and dogs), military marching, girls in an examination room | No | Vertigo, ataxic gait | Resolved in 1 week |
| Serra et al.24 | Male | 68 | Posterior | Right | Ischemic stroke | Acute | Animals and men’s head | No | Left hemiparesis, paraesthesias | Not reported |
| Inzelberg et al.25 | Female | 75 | Unspecified | Left | Ischemic stroke | 2–3 days | No | Musical hallucination of popular songs from her youth | Right hemiparesis and dysphasia | Improved with no reported treatment |
| Noda et al.26 | Male | 72 | Dorsomedial | Right | Ischemic stroke | 3 days | Vivid recollection of his old job, dish of sweet potatoes and cigarette between his fingers | No | Hypersomnolence and nocturnal insomnia | Resolved over 2 weeks with no reported treatment |
| Female | 46 | Anterior | Left | Ischemic stroke | 4 days | Parents who passed away 10 years ago, teapot and teacups on a table | Commanding voice: “Don’t eat” | Memory impairment, right upper limb weakness | Resolved over 2 weeks with no reported treatment | |
| Manford and Anderson27 | Male | 58 | Pulvinar | Right | Ischemic stroke | 10 days | Ball of light, a man in a suit, a black butterfly, dwarves, striped fish swimming | No | No | Not reported |
| Yoshida et al.28 | Female | 73 | Dorsomedial | Left | Ischemic stroke | 2 months | No | Voices telling her about misfortunes, voices of threats and commands, | Anterograde and retrograde amnesia | Risperidone and olanzapine |
| Mollet et al.29 | Female | 61 | Lateral | Right | Ischemic stroke | Acute | College-age boys in colorful Hawaiian shirts, men in black religious clothes | Conversation between college boys | Pain and numbness at the left hemibody | Not reported |
| Güzelcan et al.30 | Male | 46 | Unspecified | right | Tumor | Not reported | Parades of people, seeing spiders, mice running | No | No | Risperidone |
| Mittal and Khan31 | Female | 19 | Ventroanterior | Left | Ischemic stroke | Acute | No | Commanding Voices | Confusion, flat affect, imaginary boyfriend, and paranoid delusion | Risperidone |
| Lee et al.32 | Male | 20 | Anterior | left | Ischemic stroke | Acute | Dangerous hands and snakes | No | Amnesia, anomia, and depersonalization | Not reported |
| Fornazzari et al.12 | Male | 45 | Lateral and posterior | Left | Hemorrhage | 9 months | Sound-tactile, sound-color, and grapheme-gustatory synesthesias | No | Not reported | |
| Delgado and Bogousslavsky33 | Male | 61 | Dorsomedial | Left | Ischemic stroke | Acute | Body distortion above the waist, lights and mice running down the wall | No | Transient perioral and left paresthesias | Disappeared without treatment |
| Female | 48 | Paramedian | Right and Left (right >left) | Ischemic stroke | Acute | No | Voice and noise distortion made by “dinosaurs” | Disorientation | Disappeared without treatment | |
| Julayanont et al. (current case) | Male | 55 | Dorsomedial and pulvinar | Right | Hemorrhage | 12 months | Transient texts on his phone, unknown people and colorful airplanes | Musical hallucination | Paranoid delusions and amnesia | Risperidone |
TABLE 2. Cases With Isolated Thalamic Damage Causing Hallucinations
Even though visual hallucination is the classic type of peduncular hallucinosis, auditory hallucinations also occur after diencephalic damage. To our knowledge, there have been only two case reports of combined visual and auditory hallucinations secondary to isolated thalamic lesions, which involved the anterior and lateral nuclei in each case. Our case is the first report of damage to the dorsomedial and pulvinar nuclei contributing to combined hallucinations.
Network Model of Mania and Hallucinations Secondary to Thalamic Insults
Mania secondary to diencephalic lesions derives from the phenomenon of diaschisis that is caused by disconnection of the thalamus from the thalamo-prefrontal-limbic networks. The magnocellular (medial) part of the dorsomedial nucleus connects the thalamus with the limbic system via the orbitofrontal cortex.1 Damage to this network causes disinhibition of inappropriate behaviors and enhanced reward-seeking behaviors.2 The medial part of the dorsomedial nucleus also projects the neuronal network to the amygdala via the amygdalofugal tract, and thus a lesion on this nucleus can lead to emotional dysregulation, aggression, increased oral intake, and hypersexuality. In addition, damage to the intermediate part of dorsomedial nucleus, which links to the dorsolateral prefrontal cortex, can contribute to executive dysfunction.
Damage to the anterior nucleus, which is connected to the mammillary bodies and amygdala via the mamillothalamic and ventral amygdalothalamic tract, respectively, causes problem with emotional expression and dysregulation of motivation.1 The pulvinar nucleus is an associative nucleus connecting to multiple cortical areas.1 The medial part of the pulvinar nucleus sends some connections to the anterior insular cortex and functions in controlling emotional awareness that is required for emotional regulation.3 Some fibers from the intermediate part of the pulvinar nucleus also project to the dorsolateral prefrontal cortex and take part in executive performance.
The role of the right thalamus in the pathogenesis of mania is supported by previous studies demonstrating decreased right thalamic volume in patients with bipolar disorder compared with normal controls4,5 and reduced right thalamic and ipsilateral prefrontal/orbitofrontal perfusion in cases with diencephalic mania.6–8 It is hypothesized that emotional regulation is lateralized, with the right hemisphere controlling negative moods and the left hemisphere controlling positive emotions. The interhemispheric imbalance, with left-sided hyperfunction and right-sided hypofunction, on the prefrontal, orbitofrontal, and insular cortices, may contribute to the emotional releasing effect from the contralesional side and result in secondary mania.9,10
Similar to mania, the diaschisis of neural networks also explains the pathogenesis of peduncular hallucinosis. In the classic peduncular hallucinosis from mesencephalic lesions, the disruption along the pathway from the ascending reticular activating system in the brainstem to the thalamus may contribute to the hallucinations. While in the cases with thalamic lesions, dysregulation between the thalamus and the extrastriate cortex and superior temporal gyrus leads to visual and auditory hallucination, respectively. This hypothesis is supported by a study on the lesion-based resting-state networks, which showed the maximal network overlap for visual hallucinations on the extrastriate visual cortex and for auditory hallucinations on the superior temporal gyrus.11
The pulvinar nucleus is the multimodal integrative nucleus connecting to the posterior parietal, superior temporal, and extrastriate cortices. Damage to this structure may also cause problems with somatosensory-auditory-visual integration, resulting in multimodal hallucinations. The lateral posterior nucleus was reported to cause multimodal somatosensory-visual-auditory-gustatory synesthesia.12
We propose the network explaining the pathogenesis of mania and peduncular hallucinosis secondary to thalamic lesions (see Figure 2).
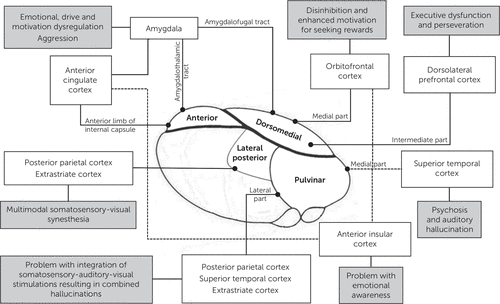
FIGURE 2. Proposed Network of Mania and Peduncular Hallucinosis Secondary to Thalamic Lesions
1 : Vascular syndromes of the thalamus. Stroke 2003; 34:2264–2278Crossref, Medline, Google Scholar
2 : Anatomical correlates of reward-seeking behaviours in behavioural variant frontotemporal dementia. Brain 2014; 137:1621–1626Crossref, Medline, Google Scholar
3 : How do you feel--now? The anterior insula and human awareness. Nat Rev Neurosci 2009; 10:59–70Crossref, Medline, Google Scholar
4 : Gray and white matter trajectories in patients with bipolar disorder. Bipolar Disord 2016; 18:52–62Crossref, Medline, Google Scholar
5 : Thalamic volumes in patients with bipolar disorder. Eur Arch Psychiatry Clin Neurosci 2010; 260:601–607Crossref, Medline, Google Scholar
6 : Manic delirium and frontal-like syndrome with paramedian infarction of the right thalamus. J Neurol Neurosurg Psychiatry 1988; 51:116–119Crossref, Medline, Google Scholar
7 : Mania caused by a diencephalic lesion. Neuropsychologia 2002; 40:245–252Crossref, Medline, Google Scholar
8 : Late-onset bipolar disorder following right thalamic injury. Actas Esp Psiquiatr 2009; 37:233–235Medline, Google Scholar
9 : Increased left anterior insular and inferior prefrontal activity in post-stroke mania. BMC Neurol 2012; 12:68Crossref, Medline, Google Scholar
10 : Left frontotemporal hyperperfusion in a patient with post-stroke mania. Psychiatry Res 2005; 139:263–267Crossref, Medline, Google Scholar
11 : Network localization of neurological symptoms from focal brain lesions. Brain 2015; 138:3061–3075Crossref, Medline, Google Scholar
12 : “Blue is music to my ears”: multimodal synesthesias after a thalamic stroke. Neurocase 2012; 18:318–322Crossref, Medline, Google Scholar
13 : Secondary mania with focal cerebrovascular lesions. Am J Psychiatry 1984; 141:1084–1087Crossref, Medline, Google Scholar
14 : Bilateral paramedian thalamic artery infarcts: report of eight cases. J Neurol Neurosurg Psychiatry 1987; 50:900–909Crossref, Medline, Google Scholar
15 : Manic-depressive and pure manic states after brain lesions. Biol Psychiatry 1991; 29:149–158Crossref, Medline, Google Scholar
16 : Hemiballismus and secondary mania following a right thalamic infarction. Neurology 1993; 43:1422–1424Crossref, Medline, Google Scholar
17 : Thalamo-frontal psychosis. Br J Psychiatry 1993; 163:113–115Crossref, Medline, Google Scholar
18 : Frontal-type memory impairment associated with thalamic damage. Int J Neurosci 1994; 77:187–198Crossref, Medline, Google Scholar
19 : Persistent recurrence of hypomania and prosopoaffective agnosia in a patient with right thalamic infarct. Neuropsychiatry Neuropsychol Behav Neurol 1998; 11:40–44Medline, Google Scholar
20 : Anosognosia and mania associated with right thalamic haemorrhage. J Neurol Neurosurg Psychiatry 2000; 68:107–108Crossref, Medline, Google Scholar
21 : Acute mania and hemichorea. Clin Neuropharmacol 2001; 24:300–303Crossref, Medline, Google Scholar
22 : Post-stroke mania: a rare but treatable presentation. Prog Neurol Psychiatry 2014; 18:24–25Crossref, Google Scholar
23 : ‘Peduncular hallucinosis’ following paramedian thalamic infarction. Neurology 1989; 39:1535–1536Crossref, Medline, Google Scholar
24 : Peduncular hallucinosis associated with posterior thalamic infarction. J Neurol 1992; 239:89–90Crossref, Medline, Google Scholar
25 : Transient musical hallucinosis. J Neurol Neurosurg Psychiatry 1993; 56:833Crossref, Medline, Google Scholar
26 : Thalamic experiential hallucinosis. J Neurol Neurosurg Psychiatry 1993; 56:1224–1226Crossref, Medline, Google Scholar
27 : Complex visual hallucinations: Clinical and neurobiological insights. Brain 1998; 121:1819–1840Crossref, Medline, Google Scholar
28 : [A case of left dorsomedial thalamic infarction with unilateral schizophrenia-like auditory hallucinations]. Seishin Shinkeigaku Zasshi 2006; 108:31–41Medline, Google Scholar
29 : Asymmetry in the emotional content of lateralised multimodal hallucinations following right thalamic stroke. Cogn Neuropsychiatry 2007; 12:422–436Crossref, Medline, Google Scholar
30 : Peduncular hallucinosis caused by a tumour in the right thalamus: A case study. Tijdschr Psychiatr 2008; 50:65–68Medline, Google Scholar
31 : Starvation causes acute psychosis due to anterior thalamic infarction. South Med J 2010; 103:701–703Crossref, Medline, Google Scholar
32 : Visual hallucinations following a left-sided unilateral tuberothalamic artery infarction. Innov Clin Neurosci 2011; 8:31–34Medline, Google Scholar
33 : ‘Distorteidolias’—fantastic perceptive distortion: A new, pure dorsomedial thalamic syndrome. Eur Neurol 2013; 70:6–9Crossref, Medline, Google Scholar



