Corticobasal Syndrome Due to Superficial Siderosis Caused by Thalamic Cavernoma
To the Editor: The classic clinical syndrome of superficial siderosis (SS) is characterized by progressive hearing loss, ataxia, and pyramidal signs, but other manifestations such as dementia may occur.1 Here we report a unique case of SS in a patient with progressive symptoms of corticobasal syndrome (CBS)2 caused by a cavernoma in the thalamus under the wall of the third ventricle.
Case Report
A 56-year-old right-handed woman with a history of hypertension was admitted to our department for consultation because of slowly worsening forgetfulness and word-finding problems started 1 year before her examination. She had a 2-year long history of severe headache episodes lasting approximately 2–3 weeks and occurring roughly three times in 1 year. During her previous consultations, she was diagnosed with migraine. Repeated brain CT scans showed progressive dilatation of the ventricular system without periventricular hypodensity (not shown). Repeated lumbar CSF puncture tests were performed without improvement of the symptoms; results on CSF tests were reported to be normal.
During her first examination in our department, alexia, apraxia, agrammatism of the speech with mild anomia, executive dysfunction (decreased category-specific verbal fluency and concretization), hypokinesis with mild right upper limb rigidity, and postural instability and wide-based gait with decreased right upper limb synkinesis were seen. The Mini-Mental State Examination (MMSE) score was 26/30 points, the Addenbrooke’s Cognitive Examination (ACE) score was 79/100 points, and the Rey-Osterrieth Complex Figure Test score was 36/36 points in the copying exercise test and 19.5/36 in the evocative test. The Syndrom-Kurztest (SKT) results were over the average: immediate evocation was 11/12 points, whereas delayed evocation was 10/12 points. No response for levodopa substitution (200 mg t.i.d.) was seen.
On the basis of the symptoms and no response to levodopa, our patient's condition was clinically diagnosed as CBS fulfilling even its most recent criteria.3
To define the pattern of the atrophy and to rule out CSF circulation problems, MR imaging was indicated. A cavernoma under the ventricular wall in the right thalamus with signal changes suggestive of SS was found (Figure 1 [A–C]). The cavernoma was removed by way of a contralateral precentral parasagittal craniotomy after the third ventricle was opened through the corpus callosum without bleeding or any other surgical complication. Results on neuropathological examination showed aberrant vascular structures with hemosiderin deposition and gliosis (Figure 1 [D and E]). Complete removal of the cavernoma was seen on the postoperative MR imaging scans with a small subependymal ischemic lesion around the cavernoma bed in the right thalamus (Figure 1 [F and G]).
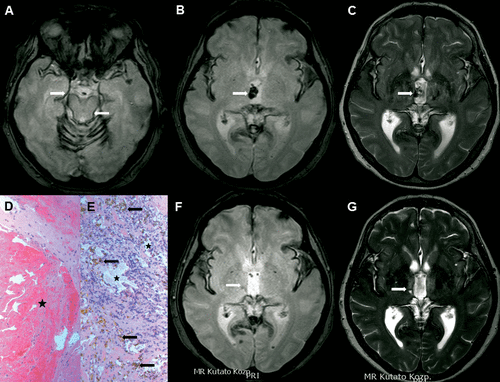
FIGURE 1. Preoperative (A–C) and Postoperative (F, G) MR Images Together With Histological Findings (D, E)a
aThe hypointense subpial rim around the medial temporal structures and the pons (arrows, A) and the right-sided thalamic cavernoma (arrow, B) are seen on T2*-weighted gradient echo MR images. The cavernoma is protruding into the third ventricle (arrow, C, T2-weighted image). Large, partially thrombotized atypical blood vessels (asterisk, D) and veinlike structures (asterisks, E) surrounded by hemosiderin depositions (arrows, E) are seen in the cavernoma removed during surgery. Postoperative MR images showing minimal subependymal signal loss on T2*-weighted gradient echo (arrow, F) and increased signal on T2-weighted images (arrow, G) in the right thalamus at the cavernoma bed.
Slight improvement of the patient's neuropsychological symptoms was seen 2 weeks after the surgery. She scored 28/30 points on the MMSE and 83/100 points on the ACE. In SKT, immediate evocation was 10/12 points, whereas delayed evocation was 8/12 points. These results did not change at 14 and 24 months after the surgery.
Discussion
Cavernous angiomas represent approximately 9% of all vascular malformations located most frequently in the cerebral hemispheres; the posterior fossa, basal ganglia, or ventricular walls are less frequently affected, whereas thalamic cavernomas are rare.4 Because of the location of thalamic cavernomas, surgical removal is difficult and comes with frequent complications, because of critical neurological functions of the thalamus and the surrounding structures. However, in a recent study complete resection was achieved in 26 patients (96.3%) without surgical mortality and 77% of the patients improved after the surgery.5
The main surgical indications are severe focal symptoms, recurrent bleeding, and progressive growth of the lesion. In our patient, the resulting SS caused progressive loss of brain tissue indicated by ventricular dilatation without signs of periventricular CSF penetration. Repeated headache periods were misdiagnosed as migraine attacks, and subarachnoid hemorrhages were not detected even by CSF examination. The small periventricular thalamic cavernoma was mistakenly not described on repeated CT scans. Because of the slowly progressive cortical symptoms with mild asymmetric parkinsonism, the clinical symptoms resembled those of CBS.
The term CBS was introduced2 to reflect the heterogeneity of the clinical symptoms and the varying underlying pathology. In most of the well-known sets of criteria, the symptoms in our patient are common (rigidity, cortical motor, and cognitive features [speech and language impairments, executive dysfunction]) and these fulfill the criteria,6 even the most recent one.3 Results on CT scans showed atrophy without other underlying pathology, and MR imaging scans defined the cavernoma and the consequent SS causing the clinical syndrome, highlighting the need for MR imaging in cases of atypical dementia.
1 : Superficial haemosiderosis of the central nervous system. J Neurol Neurosurg Psychiatry 1964; 27:332–339Crossref, Medline, Google Scholar
2 : Corticobasal degeneration and its relationship to progressive supranuclear palsy and frontotemporal dementia. Ann Neurol 2003; 54(Suppl 5):S15–S19Crossref, Medline, Google Scholar
3 : Criteria for the diagnosis of corticobasal degeneration. Neurology 2013; 80:496–503Crossref, Medline, Google Scholar
4 : Thalamic cavernous malformations. Surg Neurol 2000; 53:30–39, discussion 39–40Crossref, Medline, Google Scholar
5 : Surgical treatment and long-term outcomes of thalamic cavernous malformations. World Neurosurg 2013; 79:704–713Crossref, Medline, Google Scholar
6 : Diagnostic criteria for corticobasal syndrome: a comparative study. J Neurol Neurosurg Psychiatry 2012; 83:405–410Crossref, Medline, Google Scholar



