Disorganized Symptoms and Executive Functioning Predict Impaired Social Functioning in Subjects at Risk for Psychosis
Abstract
Predictors of social functioning deficits were assessed in 22 individuals “at risk” for psychosis. Disorganized symptoms and executive functioning predicted social functioning at follow-up. Early intervention efforts that focus on social and cognitive skills are indicated in this vulnerable population.
Schizophrenia is a chronic illness that manifests in late adolescence or early adulthood and is often preceded by both a premorbid and a prodromal phase. Unlike the premorbid phase, which is a period of relatively stable social and cognitive deficits,1 the prodromal period is characterized by its lack of stability and a downhill course of psychosocial impairment, culminating in the onset of frank psychosis.2,3
Poor social functioning at initial assessment has been implicated as an ominous sign in subjects at risk for psychosis. It has been shown that decline in social functioning before ascertainment is associated with later conversion to psychosis.4
Dysfunction in multiple cognitive domains has been reported in patients with schizophrenia as well as in individuals at risk for psychosis.5–7 The neuropsychological impairments in at-risk individuals tend to be associated with poor social and role functioning, and may predict the development of later psychosis.6–8
Despite the intuitive significance of deficits in social functioning and their importance in prodromal research, there is a dearth of longitudinal studies to explore social functioning at outcome. The present study is an attempt to elucidate the relationship between clinical symptomatology and neurocognition at initial presentation, and social functioning 1 year after ascertainment in subjects at risk for psychosis.
METHODS
Participants
The Cognitive Assessment and Risk Evaluation (CARE) program at the University of California, San Diego, provides longitudinal assessment of individuals who are considered to be at risk for developing psychosis.9 For this study, we selected a subsample (N=22) of at-risk subjects from previously published reports6,10,11 who had received the Social Adjustment Scale-Self-Report (SAS-SR) at 1-year follow-up.
Procedure
All participants received a comprehensive clinical and neurocognitive battery at initial assessment.6 The clinical assessment included the Structured Clinical Interview for DSM-IV Axis I Disorders (SCID) and the Structured Interview for Prodromal Syndromes (SIPS).12
The SAS-SR was administered to all participants at baseline assessment and at 1-year follow-up. Domains related to work/school role and social/leisure time were examined. We did not examine the two SAS-SR family domains (family unit and family outside of the home) because of the young age of our sample.
The neurocognitive battery6,11 included the Wisconsin Card-Sorting Test (WCST), the Stroop Color–Word Test, the Numerical Attention test, the Hopkins Verbal Learning Test (HVLT), Revised, the Spatial Span subtest of the Wechsler Memory Scale, 3rd Edition, as well as the Letter Number Sequencing, Block Design, and Vocabulary subtests of the WAIS, 3rd Edition.
Statistical Analyses
Analyses were performed with SPSS. Change in symptom severity and social functioning over time was assessed via paired-samples t-tests. We performed correlations between follow-up social functioning measures and baseline clinical and neurocognitive batteries to determine which variables should be included in regression analyses (with significance at p<0.05). Backward multiple-regression analyses were then performed using baseline social functioning, clinical, and neurocognitive variables as predictors of follow-up social functioning. The assumptions of normality, linearity, and homoscedasticity of residuals were met. With the use of a p<0.001 criterion for Mahalanobis distance, no outliers among the cases were found. No cases had missing data, and no suppressor variables were found (N=22).
RESULTS
Sample Characteristics
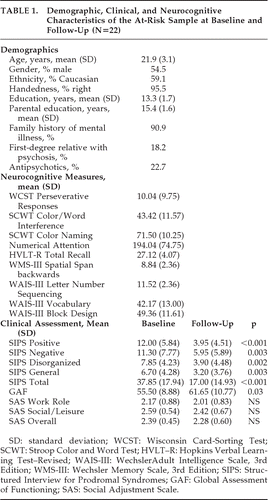
The baseline demographic characteristics and neurocognitive scores of our sample are presented in Table 1. The rate of transition to psychosis in our sample was 9.1%; two subjects converted to schizophrenia over the 1-year follow-up.
 |
Change in Clinical Symptomatology and Level of Social Functioning Over Time
As shown in Table 1, paired-samples t-tests showed significant improvement between baseline and follow-up on the Global Assessment of Functioning (GAF) and all of the SIPS ratings. However, there were no significant changes over time on any of the SAS-SR ratings. The at-risk subjects remained impaired in their social functioning at follow-up.
Prediction of Social-Functioning Outcomes
Given our relatively small sample size, we limited the number of predictor variables that were used in the regression analyses to those that had significant correlations (p<0.05) with the social functioning variables at follow-up (r=0.45 to 0.67). Yet, for each dependent variable, the corresponding baseline variable was entered into the prediction model regardless of the magnitude of the correlation between them. Interestingly, the outcome social-functioning measures were not significantly correlated with baseline GAF, SIPS positive symptoms, or performance on the WCST. In order to avoid multicollinearity problems, we examined the correlations among the predictor variables. Those correlations were all small-to-moderate (r=0.43 to 0.59; p<0.05) except for the high association between SIPS Disorganized and SIPS Negative (r=0.71; p<0.001).
We decided to include both of those variables in the regression analyses because they represent different symptom domains. We performed three backward multiple-regression analyses, one for each SAS outcome variable.
When the four variables that were significantly correlated with follow-up, Overall SAS, in addition to baseline Overall SAS scores, were included in the first backward multiple regression; we observed a significant regression coefficient that accounted for 70% of the variance in overall functioning at outcome: F[5, 15]=7.18; p=0.001; R2=0.70 (at Step 1). After Stroop Color Naming and SIPS Negative were excluded from the model, baseline Overall SAS, SIPS Disorganized, and Stroop Color/Word Interference still accounted for 70% of the variance in follow-up Overall SAS: F[3, 17]=13.29; p<0.001; R2=0.70 (at Step 3). The most significant predictor of overall functioning was SIPS Disorganized (β=0.59), followed by Stroop Color/Word Interference (β = –0.44). Baseline SAS Overall was not a significant predictor (β=0.28; p=0.06).
When the four variables that were significantly correlated with follow-up SAS Social/Leisure, in addition to baseline SAS Social/Leisure, were included in the second backward multiple regression, we observed a significant regression coefficient that accounted for 64% of the variance in social role functioning at outcome: F[5, 15]=5.42; p=0.005; R2=0.64 (at Step 1). After SAS Social/Leisure and SIPS Negative were excluded from the model, the three-predictor model, including SIPS Disorganized, HVLT Total Recall, and Stroop Color/Word Interference, accounted for 61% of the variance in follow-up SAS Social/Leisure, F[3, 17]=8.78; p=0.001; R2=0.61 (at Step 3). The most significant predictor of social role functioning was SIPS Disorganized (β=0.49), followed by the Stroop Color/Word Interference (β = –0.37). HVLT's regression coefficient was not significant (β = –0.31; p=0.08).
When the three variables that were significantly correlated with follow-up SAS Work Role, in addition to baseline SAS Work Role, were included in the third backward multiple regression, we observed a significant regression coefficient that accounted for 81% of the variance in Work Role Functioning at outcome: F[4, 11]=11.62; p=0.001; R2=0.81 (at Step 1). After baseline SAS Work Role was excluded from the model, Stroop Color-Naming, Stroop Color/Word Interference, and Numerical Attention significantly contributed to the prediction of follow-up SAS Work Role, accounting for 79% of the variance: F[3, 12]=14.92; p<0.001; R2=0.79 (at Step 2). The most significant predictor of follow-up Work Role Functioning was Stroop Color-Naming (β = –0.50), followed by the Stroop Color/Word Interference (β = –0.38), and Numerical Attention (β=0.31).
DISCUSSION
Our results showed that disorganized symptoms and executive functioning deficits at baseline assessment were significant predictors of overall social functioning and the subscale of social role functioning. Work role impairment was also accounted for by deficits in executive functioning, as well as processing speed.
Impairment in social functioning is arguably the most debilitating aspect of schizophrenia, in the broader context of an individual's lifelong struggle with the disorder. Interestingly, our results indicate that longitudinal outcomes of social functioning impairment are independent of positive symptoms. This finding is noteworthy, as it suggests that regardless of successful treatment of positive symptoms, individuals at risk for schizophrenia continue to have social functioning deficits.13,14 Therefore, assessment of and early intervention for impairments in social functioning are unquestionably important in this population.
This finding, if corroborated by larger studies, suggests that interventions addressing social functioning in this vulnerable group are indicated. Social skills training, individualized educational programs, and family psychoeducation and/or psychotherapy could all help reduce stress and improve functional outcome. Also, psychosocial treatment efforts that focus on cognitive training or remediation might help to ameliorate the observed functional deficits in this vulnerable group.14,15
1. : Behavioral and intellectual markers for schizophrenia in apparently healthy male adolescents. Am J Psychiatry 1999; 156:1328–1335Medline, Google Scholar
2. : The diagnosis of schizophrenia: a review of onset and duration issues. Schizophr Bull 1991;17: 51–67Crossref, Medline, Google Scholar
3. : Monitoring and care of young people at incipient risk of psychosis. Schizophr Bull 1996; 22: 283–303Crossref, Medline, Google Scholar
4. : Prediction of psychosis in youth at high clinical risk: a multisite longitudinal study in North America. Arch Gen Psychiatry 2008; 65:28–37Crossref, Medline, Google Scholar
5. : Neuropsychological change in young people at high risk for schizophrenia: results from the first two neuropsychological assessments of the Edinburgh High-Risk Study. Psychol Med 2000; 30:1111–1121Crossref, Medline, Google Scholar
6. : Neurocognitive deficits in the (putative) prodrome and first episode of psychosis. Schizophr Res 2007; 93:266–277Crossref, Medline, Google Scholar
7. : Neurocognitive performance and functional disability in the psychosis prodrome. Schizophr Res 2006; 84:100–111Crossref, Medline, Google Scholar
8. : The course of neurocognition and social functioning in individuals at ultra high risk for psychosis. Schizophr Bull 2007; 33:772–781Crossref, Medline, Google Scholar
9. : How does studying schizotypal personality disorder inform us about the prodrome of schizophrenia? Curr Psychiatry Reports 2005; 7:41–50Crossref, Medline, Google Scholar
10. : Social functioning in young people at risk for schizophrenia. Psychiatry Res 2007; 151:29–35Crossref, Medline, Google Scholar
11. : Course of neurocognitive deficits in the prodrome and first episode of schizophrenia. Neuropsychology 2010; 24:109–120Crossref, Medline, Google Scholar
12. : Prodromal assessment with the structured interview for prodromal syndromes and the scale of prodromal symptoms: predictive validity, interrater reliability, and training to reliability. Schizophr Bull 2003; 29:703–715Crossref, Medline, Google Scholar
13. : The schizophrenia prodrome revisited: a neurodevelopmental perspective. Schizophr Bull 2003; 29:633–651Crossref, Medline, Google Scholar
14. : Risk and protection in prodromal schizophrenia: ethical implications for clinical practice and future research. Schizophr Bull 2003; 32:166–178Crossref, Google Scholar
15. : Patterns of premorbid functioning in first-episode psychosis: relationship to 2-year outcome. Acta Psychiatr Scand 2005; 112:40–46Crossref, Medline, Google Scholar



