Auditory Hallucinations as the Only Presenting Symptom of Right-Parietal Spontaneous Hemorrhage: FDG-PET Evidence of Corpus Callosum Hyperactivity
Case Report
A 67-year-old woman was admitted to the emergency room of our hospital for acute onset of complex auditory hallucinations; she reported hearing loud music and voices of known persons speaking “filthy.” She had never suffered any psychiatric disorders in the past, and she was taking atenolol for many years as the only treatment for chronic arterial hypertension.
Neurological examination did not show any focal neurological signs, and blood tests were normal. Brain CT scan revealed a right-parietal hemorrhage involving both superficial and deep territory of the posterior branches of middle cerebral artery (Figure 1 [D]). EEG showed absence of focal paroxystic epyleptiform discharges. Brain MRI and MR-angio confirmed the intraparenchimal hemorrhage, excluding the presence of aneurysm or artero-venous malformations. FDG-PET scan showed a significant increase in glucose metabolism (versus normal control database) in the middle and posterior areas of corpus callosum as well as in the precuneus and cuneus cortex (Figure 1 [A, B, C]).
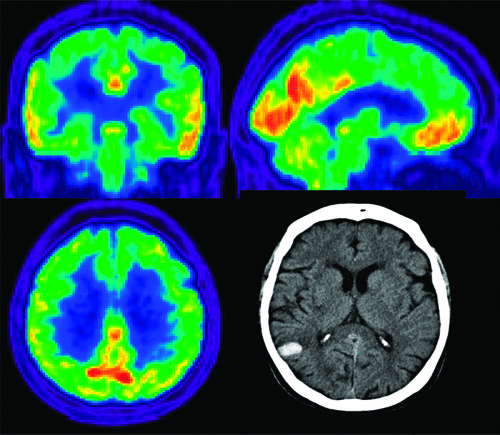
The auditory hallucinations gradually resolved in a few days without any treatment. She was discharged after 18 days from onset, and neurological examination showed visuospatial deficit as the consequence of right-parietal damage.
Discussion
Auditory hallucinations are uncommon phenomena in patients with acute stroke; in particular, they have been reported in acute ischemic lesions of the brainstem but very rarely reported after cortical ischemic strokes.1 To our knowledge, this is the first case of auditory hallucinations as the only presenting symptom of a spontaneous hypertensive parenchymal hemmorrhage.
In our case FDG-PET scan showed high relative glucose metabolic rates in the middle and posterior areas of corpus callosum. Hyperactivity of corpus callosum has already been reported in schizophrenic patients with auditory hallucinations.2,3 In particular, abnormalities in the posterior part of corpus callosum has been associated to schizophrenic positive symptoms.4 We speculate that in our patient the acute cortico-subcortical hemorrhage caused, through rapid development of peri-lesional edema and release of excitatory mediators such as calcium ions and amino-acids, an electrode-like effect,5 which abnormally activated the posterior part of corpus callosum, with consequent development of auditory hallucinations. We believe that a better understanding of corpus callosum pathophysiology could help in clarifying the mechanism of perceptive disturbances of various origin.
1. : Auditory hallucinations in acute stroke. Behav Neurol 2005; 16:211–216Crossref, Medline, Google Scholar
2. : Relative glucose metabolic rate higher in white matter in patients with schizophrenia. Am J Psychiatry 2007; 164:1072–1081Crossref, Medline, Google Scholar
3. : Pathways that make voices. Arch Gen Psychiatry 2004; 61:658–668Crossref, Medline, Google Scholar
4. : Reduced interhemispheric connectivity in schizophrenia: tractography base segmentation of the corpus callosum. Schizophr Res 2008; 106(2–3):125–131Crossref, Medline, Google Scholar
5. : White-matter glucose metabolism during intracortical electrostimulation: a quantitative fluorodeoxyglucose autoradiography study in the rat. Neuroimage 2002; 16:993–998Crossref, Medline, Google Scholar



