Duloxetine's Effects in Resting Functional Magnetic Resonance Imaging of First-Episode, Drug-Naïve Major Depressive Disorder With Panic Disorder Patients
Case Report
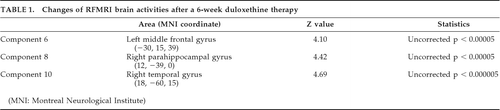
Two cases (1 woman, and 1 man; 28 and 18 years old, respectively) with first-onset, drug naïve MDD with PD were enrolled. They all received clinical rating scales, with scores as follows: Hamilton Rating Scale for Depression (Ham-D): 30, 24; and Panic Disorder Severity Scale (PDSS): 20, 18. The treatment with duloxetine 30 mg/day was started and titrated to 60 mg within 2 weeks without any significant side effects except mild nausea and sedation. After a 6-week therapy, their MDD and PD symptoms responded to duloxetine [Ham-D: 4, 5; PDSS: 2, 1]. RFMRI scans were obtained with a 3T GE version scanner. Echo planar imaging (EPI) sequences were acquired in 20 axial slices (TR=2,000 msec, TE=40 msec, flip angle=90°, FOV=24 cm; 5-mm thickness and 1 mm gap; 400 sec for each subject) at baseline and 6th week visit. RFMRI data were first preprocessed by DPARSF (Data Processing Assistant and Resting-State FMRI, Version 1.4), which included slice timing, realignment, normalization, smoothing by 4 × 4 × 4 kernel, detrend and filter RFMRI, with data within 0.008–0.08 Hz. The preprocessed RFMRI data were then processed by GIFT (Group Independent Component Analysis of FMRI Toolbox, Version 1.3 hour), and subsequently compared analysis between baseline and the 6th week (uncorrected p<0.00005; voxel threshold >50). There were modest increases of RFMRI brain activities after duloxetine treatment (Table 1).
 |
Discussion
Limbic and paralimbic activations usually inhibit the activities of dorsal cortical structures (such as middle frontal gyrus) in MDD patients.1 Remitted MDD patients have been reported with increased regional homogeneity in frontal areas.2 Liao et al.3 found that decreased dorsal attentional network in middle frontal gyrus with hyperactive episodic-memory and self-projection network in temporal and parahippocampal gyrus probably contributed to the anxiety and panic attacks. Also, the increased vigilance and autonomic, visceral dysregulations due to abnormal activities of RFMRI in these regions4 should be associated with panic symptoms in these patients.
1. . Investigating neural primacy in major depressive disorder: multivariate Granger causality analysis of resting-state fMRI time-series data. Mol Psychiatry 2010Medline, Google Scholar
2. : Abnormal neural activity in the patients with remitted geriatric depression: a resting-state functional magnetic resonance imaging study. J Affect Disord 2008; 111:145–152Crossref, Medline, Google Scholar
3. : Selective aberrant functional connectivity of resting-state networks in social anxiety disorder. Neuroimage 2010; 52:1549–1558Crossref, Medline, Google Scholar
4. : Resting-state functional MRI in depression unmasks increased connectivity between networks via the dorsal nexus. Proc Natl Acad Sci U S A 2010; 107:11020–11025Crossref, Medline, Google Scholar



