Neuroanatomical Abnormalities Before the Onset of Various Types of Delusions in a Patient With Alzheimer Disease
To the Editor: Structural brain abnormalities associated with delusions in Alzheimer Disease (AD) are poorly understood. Also, whether the neural substrate underlying the delusions develops before the onset of the delusions is unclear. Here, we report on an AD patient who developed various types of delusions and who exhibited magnetic resonance imaging (MRI) findings atypical of AD before the onset of the delusions.
Case Report
The patient was a 78-year-old, married, right-handed woman. Around the age of 75 years, her family noticed episodic memory disturbances. At the age of 78 years, she visited our hospital with her family as an outpatient. She was diagnosed as probable AD according to the National Institute of Neurological and Communication Disorders and Stroke/Alzheimer’s Disease and Related Disorders Association (NINCDS/ADRDA) criteria.1 Her Mini-Mental State Exam (MMSE) score was 18/30. She did not exhibit psychotic symptoms at the time of her first visit, and she had no previous history of psychiatric disease. One year later, she developed delusions of theft associated with a delusional jealousy that her husband was having an extramarital affair and that her husband and his lover had stolen her money. Thus, risperidone (0.5 mg/day) was prescribed for her delusions, and the delusions disappeared. However, over the next 6 months, she developed delusional misidentification. She insisted that her daughter was not who she really was. The dose of risperidone was increased to 1 mg/day, which alleviated the delusional misidentification.
At the time of her first visit to our hospital, the patient’s MRI findings were analyzed, using the voxel-based specific regional analysis system for AD (VSRAD), which utilizes a voxel-based morphometry (VBM) analysis.2 Relative to normal controls, significant volume reductions were detected in not only bilateral hippocampal regions, but also bilateral insular cortex, anterior cingulate cortex, right orbitofrontal cortex, and bilateral inferior frontal cortex (Figure 1). A 78-year-old patient with probable AD who did not develop delusions but who had a similar demographic background exhibited significant volume reductions mainly in bilateral hippocampal regions, relative to normal controls. When the second MRI examination was performed after the development of the misidentification delusions, the atrophy showed more progression than that observed during the first MRI examination. The second MRI examination did not show any additional findings, such as hemorrhages.
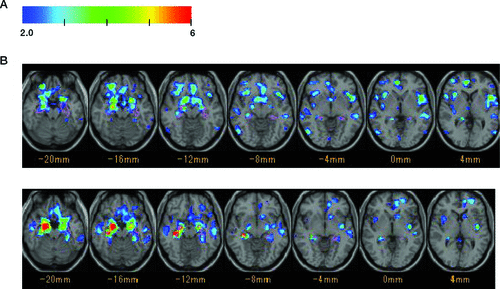
[A]: Axial VSRAD (current patient; age 78 years) shows several areas with atrophy, including bilateral insular cortices, the anterior cingulate cortex, the right orbitofrontal cortex, bilateral inferior frontal cortices, and bilateral hippocampal regions; [B]: control case (78-year-old patient with AD who did not develop delusions) mainly shows atrophy in bilateral hippocampal regions.
Discussion
The presently reported case exhibited various types of delusions during an 18-month period. Although her MRI findings showed bilateral hippocampal atrophy, other areas of atrophy, such as the bilateral insular cortex and the right orbitofrontal cortex, were also identified with VSRAD. Both the frontal and insular areas are thought to be linked with psychotic symptoms in AD patients.3,4 More importantly, before the onset of the delusions, the patient exhibited volume reductions in these areas. Thus, the abnormalities in both the frontal areas and the insulae likely reflect a pre-existing vulnerability in the present patient with AD who developed delusions. Further longitudinal study of a large sample of AD patients who develop delusions may be needed to clarify this hypothesis.
1 : Clinical Diagnosis of Alzheimer’s Disease: Report of the NINCDS-ADRDA Work Group Under the Auspices of the Dept. of Health and Human Services Task Force on Alzheimer’s Disease. Neurology 1984; 34:939–944Crossref, Medline, Google Scholar
2 . Voxel-based morphometry to discriminate early Alzheimer’s disease from controls. Neurosci Lett 2005; 382:269–274Crossref, Medline, Google Scholar
3 : Neuroanatomical correlates of neuropsychiatric symptoms in Alzheimer’s disease. Brain 2008; 131:2455–2463Crossref, Medline, Google Scholar
4 : Insular hypoperfusion correlates with the severity of delusions in individuals with Alzheimer’s disease. Dement Geriatr Cogn Disord 2010; 29:287–293Crossref, Medline, Google Scholar



