Comorbid Multiple Sclerosis and TDP-43 Proteinopathy in a Gulf War Sea Captain
Case Report
A 60-year-old deep-sea captain with a diagnosis of MS presented to the tertiary hospital for further investigations of cognitive decline. His first symptoms were temporally related by his family to an incident a decade previously when his ship caught fire during the Gulf War, and he was exposed to smoke and fumes without being able to leave the ship for weeks. After this traumatic experience, he started to complain of progressive bladder and sexual dysfunction, problems with dexterity, and gait disturbance. After investigation, he was diagnosed with MS at the age of 52. Concurrent with the development of physical symptoms, the family also noted impaired naming and word-finding difficulties, manifesting as circumlocutions in conversations. Later, more pronounced deficits in comprehension of language, object-recognition, and surface dyslexia manifested, causing great distress to the patient and his family and leading him to retire early. His visuospatial skills, phonological and syntactic processes, and, to some extent, episodic memory, were initially spared. There was no other personal or family history of note. On examination, he had mild weakness in his right lower limb, brisk reflexes, and bilateral up-going plantar responses. Blood screen, including treponemal serology, was negative, but CSF showed IgG oligoclonal bands. Neuroimaging revealed periventricular white-matter lesions, as well as asymmetric frontotemporal atrophy, more pronounced on the left, and disproportionate to the number of white-matter lesions. Neuropsychological testing showed a verbal IQ of 69 and performance IQ of 86. His verbal subtest scores ranged from extremely low (Vocabulary and Similarities) to average (Digit Span). He also had extremely low scores on the Picture Completion performance test, while scoring high-average on Matrix Reasoning. Verbal recognition was less efficient than visual recognition-memory. The possibility of a dual neurological diagnosis of MS and a frontotemporal-dementia-spectrum disorder was considered likely. He was started on galantamine, but continued to deteriorate physically, cognitively, and behaviorally over the next 3 years, necessitating residential placement, where he eventually died. Postmortem histopathological examination disclosed two distinct and separate pathologies: MS and widespread TDP-43 proteinopathy. Severe neuronal loss was found in the left temporal cortex with an anterior gradient (Figure 1 [A]). The rest of the brain showed moderate cortical atrophy, with white-matter loss. The MS mainly affected the spinal cord and brainstem (Figure 1 [B]). There were widespread TDP-43-positive dystrophic neurites, no intranuclear, and only rare intracytoplasmic inclusions in the neurones of neocortex and limbic system, in keeping with frontotemporal lobar degeneration with TPD-43 proteinopathy (FTLD-TDP43) subtype 1 (Figure 1 [C]).
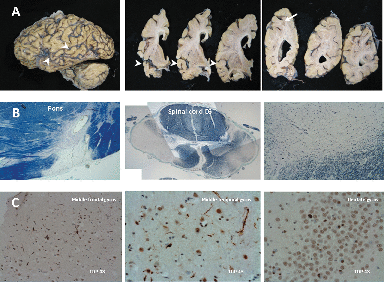
[A]The cortical atrophy is most severe, almost knife-edge, in the anterior and medial temporal lobe, whereas the posterior part of the superior temporal gyrus (arrowheads) is more preserved. There is a demyelinating plaque in the parietal lobe (arrows). [B] The demyelinating lesions of MS were all inactive (burnout) plaques and mainly affected the spinal cord and the brainstem (Luxol fast blue-Nissl). [C] There was severe neuronal loss in the temporal cortex, and less severe in the frontal lobe, accompanied by superficial microvacuolation. Widespread TDP-43-positive dystrophic neurites and only rare intracytoplasmic (mainly round) inclusions were present in the neocortex and limbic system. No obvious TDP-43-positive intranuclear inclusions were seen, and no significant TDP-43 pathology was noted in the spinal cord. No immunoreactivity against Tau, Aβ, or α-synuclein was present.
Discussion
TDP-43 proteinopathies represent a heterogeneous group of disorders, with a broad clinicopathological spectrum (i.e., from FTLD-TDP-43, at one end, to ALS, at the other) involving multiple systems and sharing similar disease mechanisms linked to pathological TDP-43.3 In sporadic cases, various environmental factors have been considered as possible triggers of the neurodegenerative cascade, including a history of trauma to the CNS (leading to axonal injury), strenuous physical activity, exposure to heavy metals, etc.4 Our patient reportedly presented with physical and cognitive symptoms shortly after being exposed to unknown toxic fumes and prolonged extreme psychophysiological stress. Although patients with MS can show early decline in cognitive functioning, this usually takes the form of difficulties with executive function.2 Here, progressive language and cognitive dysfunction was suggestive of semantic dementia (SD).5 SD is a syndrome within the spectrum of frontotemporal lobar degenerations, characterized by fluent progressive aphasia, with emphasis on anomia, and loss of word-meaning.5 SD has been recently associated with clinicopathological diagnosis of FTLD-TDP-43 subtype 1, which is in keeping with the postmortem findings in our patient.3,6 Coexisting TDP-43 pathology has been reported in several neurodegenerative diseases, but, thus far, not in MS.3,4 A random nature for this association cannot be excluded with certainty. Lately, however, axonal injury/loss has been argued to play a role in the evolution of both pathologies, and it is tempting to speculate that it also formed a common ab initio pathological substrate in the case presented here.4,7
1. : Multiple sclerosis. Lancet 2002; 359:1221–1231Crossref, Medline, Google Scholar
2. : Cognitive impairment as marker of diffuse brain abnormalities in early relapsing-remitting multiple sclerosis. J Neurol Neurosurg Psychiatry 2005; 76:519–526Crossref, Medline, Google Scholar
3. : Amyotrophic lateral sclerosis and frontotemporal lobar degeneration: a spectrum of TDP-43 proteinopathies. Neuropathology 2010; 30:103–112Crossref, Medline, Google Scholar
4. : TDP-43 proteinopathy and motor neuron disease in chronic traumatic encephalopathy. J Neuropathol Exp Neurol 2010; 69:918–929Crossref, Medline, Google Scholar
5. : Semantic dementia and primary progressive aphasia: a problem of categorization? Alzheimer Dis Assoc Disord 2005; 19:S7–S14Crossref, Medline, Google Scholar
6. : Molecular neuropathology of TDP-43 proteinopathies. Int J Mol Sci 2009; 10:232–246Crossref, Medline, Google Scholar
7. : Axonal injury in multiple sclerosis. Curr Neurol Neurosci Rep 2003; 3:231–237Crossref, Medline, Google Scholar



