Cavum Septi Pellucidi and Cavum Vergae With Increased Amyloid β Cortical Load in a 65-Year-Old Woman With Bipolar Disorder: Post-Mortem Neuropathological Observations
To the Editor: A case of a cavum septi pellucidi (CSP) and cavum vergae (CV) discovered incidentally in a 65-year-old woman with history of bipolar disorder with suicidal ideations is reported. The decedent died as a result of acute anoxic-ischemic encephalopathy of unknown etiology (patient was found unresponsive on the street). A head CT scan performed on admission to the emergency room showed a cystic space within the septum pellucidum with significant caudal extension consistent with a CSP/CV (Figure 1A). The two cava were not separated (Figure 1A). The antero-posterior length measured on CT was 5.7 cm. A follow-up head CT performed 2 days after admission demonstrated, besides the cava (Figures 1B and 1C), hypodensities in the thalamic and lentiform nuclei bilaterally consistent with hypoxic/ischemic injury (Figure 1C). Neuropathological evaluation at autopsy revealed a large CSP (Figures 2A-2C and Figures 3A) extending caudally to become CSP/CV (Figures 2D, 3B, 4A, and 4B). There was moderate dilatation of the lateral ventricles but no evidence of fenestrations in the septal leaves, pointing against a communication between the septal cavum and the lateral ventricles (Figure 3A).
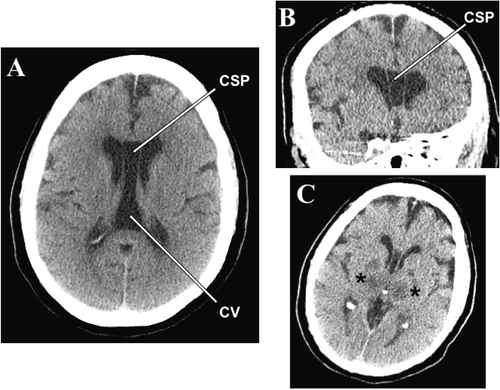
Panel A is an axial image from a noncontrast head CT scan performed upon admission demonstrating a cavum septi pellucidi (CSP) and cavum vergae (CV), both depicted by arrows, which are in communication with one another. Panels B and C are coronal and axial images respectively from a follow up noncontrast head CT performed 2 days later, shortly prior to the patient’s demise. The CSP is partially visualized in both panels. There is moderate symmetrical dilatation of the lateral ventricles with rounding of the lateral ventricular angles. Panel C also demonstrates bilateral hypodensities in the thalamus and globus pallidus (asterisks) consistent with hypoxic-ischemic damage.
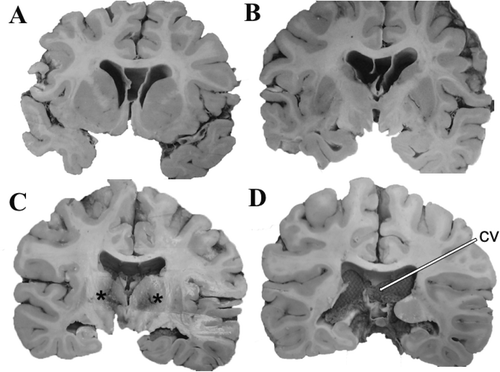
The rostrocaudal extent of the septal cavum is shown at different coronal cuts of the brain [A‒D]. Areas of thalamic necrosis are demarcated with asterisks [C]. CV is depicted by arrow in the caudal most section at the coronal level of the atrium/trigone of the lateral ventricle [D]. Note moderate dilatation of the lateral ventricles with rounding of the lateral ventricular angles [A‒D].
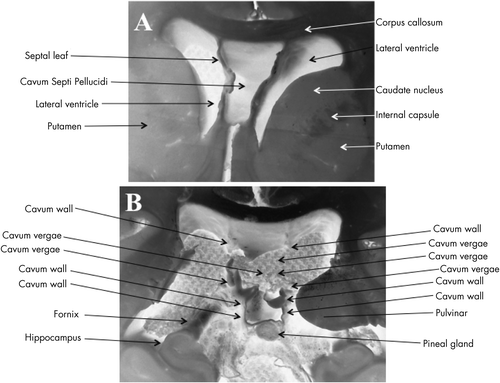
Panel A is a close up view of panel A in Figure 2 showing a large cavum septi pellucidi. Inverted images were used to better illustrate the intactness of the leaves of the septal cavum. There is lack of septal fenestrations. Panel B is a close up view of panel D in Figure 2 showing anatomical details of the cavum vergae including demonstration of one of the pillars of the fornix lateral to the cavum wall.
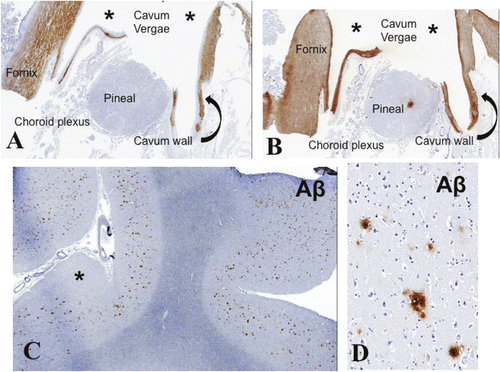
Panels A and B are low power views of histological sections from the region of the cavum vergae (asterisks) corresponding to panel B in Figure 3, immunostained with antibodies to myelin basic protein (MBP) for the delineation of myelinated fibers [A] and glial fibrillary acidic protein (GFAP) for the demarcation of glial fibers [B]. Note MBP and GFAP labeling in the wall of the cavum vergae confirming that the latter contains myelinated axons and glial fibers in a distribution similar to that in the nearby fornix. Note lack of MBP staining in the pineal gland and the choroid plexus. Expected focal GFAP labeling is noted in the pineal. Panels C and D demonstrate diffuse amyloid beta (Aβ) deposits of moderate density in the cerebral cortex (asterisk).
Diffuse hypoxic/ischemic changes were demonstrated in the hippocampus, amygdala, thalamic nuclei, and cerebral cortex consistent with cardiac arrest encephalopathy (Figures 1C and 2C). The cerebral cortex, including prefrontal cortex and hippocampus, was developmentally unremarkable. Diffuse amyloid beta (Aβ) deposits of moderate density without neuritic plaques were noted in the transentorhinal region, entorhinal cortex, cingulate cortex, and cerebral neocortex (Figures 4C and 4D). Neurofibrillary pathology was absent (lack of phosphorylated tau protein and α-synuclein immunoreactivity). The cerebral hemispheric white matter was essentially unremarkable.
The demonstration of CSP/CV in the present case may be significant given the decedent’s history of bipolar disorder with major depression, characterized by suicidal tendency. Although an association between CSP and psychosis, especially schizophrenia, is well established,1–3 the relationship between CSP/CV and affective disorders is less well known.4–7 Previous MRI studies have shown that bipolar disorder patients exhibit higher prevalence of abnormal CSP enlargement (≥6 mm in length) compared with healthy controls.6,7 The septum pellucidum, one of the substrates of “affect” in the Papez circuit,8 is an important relay station of the limbic system, transmitting visceral information through the hypothalamus to the hippocampus, amygdala, habenula, and the reticular formation of the brainstem, thus, regulating the emotional response to the environment.9 A disruption of this circuit may be further complicated by the anatomical proximity of the septal leaves to the fornix, the latter originating in the subiculum, alveus, and stratum pyramidale of the hippocampus.3 In the context of affective disorders, the functional implication of disruption of the septal connections to the anterior (subcallosal) cingulate cortex (prefrontal cortex) deserves consideration; because the septum pellucidum has a role in motivational behavior,10 an anatomical-functional disruption of this structure may contribute to the lack of motivation commonly observed in major depressive disorder. Interestingly, CSP has also been reported in catatonia.11 Catatonic behaviors may be encountered in major depression.12
To our knowledge, the occurrence of an increased Aβ cortical load has not been hitherto reported in the context of CSP/CV. Although it is possible that the two findings are merely coincidental, the relationship between cortical degeneration with resultant incipient brain atrophy, expanding CSP/CV, and worsening of psychotic manifestations is a subject of tempting speculation, as previously suggested.13 The present case provides additional neuropathological evidence for a link of CSP/CV and affective disorders.
1 : Malformations of the septum pellucidum: two distinctive cases in association with schizophrenia. J Psychiatry Neurosci 1994; 19:140–144Medline, Google Scholar
2 : Enlarged cavum septi pellucidi in patients with schizophrenia: clinical and cognitive correlates. J Neuropsychiatry Clin Neurosci 2000; 12:344–349Link, Google Scholar
3 : Cavum septum pellucidum and its increased prevalence in schizophrenia: a neuroembryological classification. J Neuropsychiatry Clin Neurosci 2004; 16:41–46Link, Google Scholar
4 : Clinical correlates of septum pellucidum cavities: an unusual association with psychosis. Psychol Med 1985; 15:43–54Crossref, Medline, Google Scholar
5 : MRI study of cavum septi pellucidi in schizophrenia, affective disorder, and schizotypal personality disorder. Am J Psychiatry 1998; 155:509–515Crossref, Medline, Google Scholar
6 : The occurrence of cavum septi pellucidi enlargement is increased in bipolar disorder patients. Bipolar Disord 2007; 9:274–280Crossref, Medline, Google Scholar
7 : Cavum septi pellucidi in first-episode schizophrenia and first-episode affective psychosis: an MRI study. Schizophr Res 2004; 71:65–76Crossref, Medline, Google Scholar
8 : A proposed mechanism of emotion. Arch Neurol Psychiatry (Chicago) 1937; 38:725–734Crossref, Google Scholar
9 : The septum pellucidum: normal and abnormal. AJNR Am J Neuroradiol 1989; 10:989–1005Medline, Google Scholar
10 : The connexions of the septum. Brain 1966; 89:317–348Crossref, Medline, Google Scholar
11 : Catatonic schizophrenia with cavum septum pellucidum. J Neuropsychiatry Clin Neurosci 2012; 24:E33Link, Google Scholar
12 : Catatonia in depression: prevalence, clinical correlates, and validation of a scale. J Neurol Neurosurg Psychiatry 1996; 60:326–332Crossref, Medline, Google Scholar
13 : Late onset of psychotic symptoms in a patient with cavum septum pellucidum and cavum vergae. J Neuropsychiatry Clin Neurosci 2012; 24:E43–E44Link, Google Scholar



